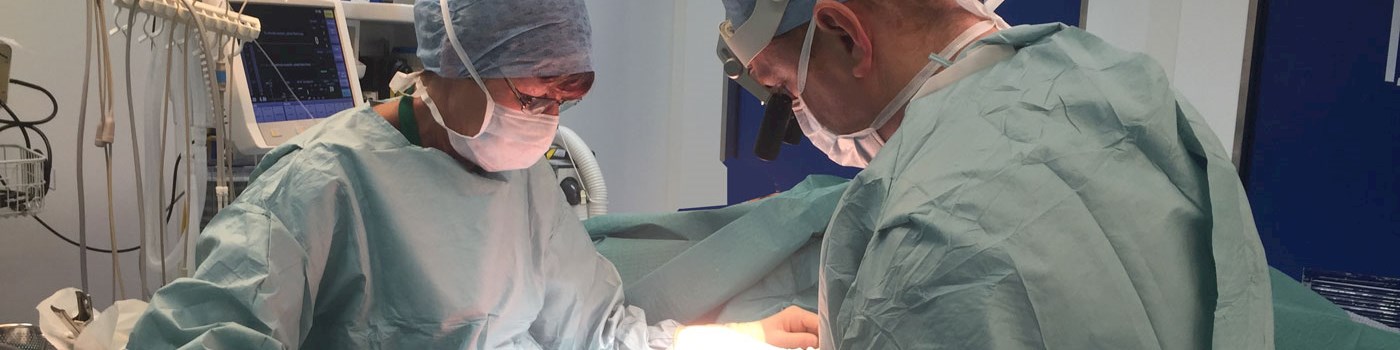
At present wrist replacements are used in post retirement patients with osteo-arthritis or patients with rheumatoid arthritis.
They are excellent in controlling pain and allow patients to maintain some movement. Traditionally wrist fusions have been undertaken when arthritis is severe, but now there is the option of wrist replacement.
However wrist replacement is not suitable for all patients. The results have shown that they will last for a shorter time than other large joint replacements such as in the knee and hip. They usually fail by loosening around 10 years. This early failure is accelerated if the patients are high demand and that is why this procedure is only recommended to low demand patients, such as those post retirement and with systemic diseases such as rheumatoid arthritis.
What are the risks?
The risks are low, but include:
- Infection – risk is low around 1%, but if it occurs it is a serious problem as control of infection can be difficult, due to the implant
- Pain – This usually settles over the first week and is usually moderate. It may be quite severe in the first 24 hours and is why you need to stay in and receive stronger painkillers.
- Stiffness – Often the joint that is being replaced is very stiff. If this is the case the resultant movement after the operation will be limited. A result with 20 degrees extension and 30 degrees flexion would be acceptable. Most activities of daily living can be undertaken with this range of movement.
- Swelling – The wrist will remain swollen for 3 to 6 months
- Nerve injury – Localised numbness around the wound may occur. It usually resolves with time. Occasionally the post-operative swelling can cause carpal tunnel syndrome. This is when the nerve passing across the front of the wrist is compressed causing pain and tingling in the thumb, index and middle finger. If this occurs a further small operation may be required to relief the pressure.
- Dislocation – This is a risk in the short term, before the tissues tighten. The risk is low, but if it does occur, a short general anaesthetic is required to relocate the joint.
- Loosening – This is the long term complication of the joint replacement and is almost inevitable. Once the joint is loose, it may become painful and swollen again. At that stage the majority of patients would have their replacement converted to a fusion. Hopefully though there have been many years of benefit!
How is the operation performed?
You will normally attend hospital on the day of surgery.
The choice of anesthetic will be discussed by the anesthetist, but may be a general anesthetic, where you are asleep, or a nerve block where your arm is numb, supplemented with sedation if required.
The procedure involves removing the arthritic diseased bone and inserting an artificial joint made of metal and plastic.
Afterwards there is a large bulky dressing, with a plaster splint. The stability of the replacement at the end of the operation will determine the speed at which you can start to regain movement and strength.
Average length of stay is one night.
After discharge you will be seen by the hand therapist and reviewed by the surgeon in the outpatient clinic around 2 weeks. Any stitches present may require to be removed then. After this point your rehabilitation will be guided by the hand therapist.
Find A Surgeon
Find a surgeon in your area.
Consent Form
You can access the consent form using the button below.